We need to stop avoiding the problem and start envisaging what will matter to us when we are older to drive a paradigm shift in the way residential aged care is provided in Australia.
We have a problem
You would have had to be living under a rock for the past few years if you have missed the plight of many residents in aged care in Australia. First the Royal Commission into Aged Care Quality and Safety and then subsequent waves of the COVID-19 pandemic confirmed the general perception of residential aged care (RAC) as a fate worse than death.
One of the things I like most about devising and leading charrettes is seeing how new solutions to old problems emerge as the collaborative process unfolds.
One of the groups I most like working with is Longevity By Design whose purpose is creating visionary and innovative design to meet the needs of future seniors.
Put these two things together and we have a passionate group of people who set out to re-imagine aged care design in the post-pandemic era at the Longevity By Design 2021 Challenge “Feels Like Home” at UQ.
This article I wrote with Prof Laurie Buys, published in The Conversation captures only a fraction of the great ideas that emerged from that process. See the teams’ 4-minute pitches and the judging panel’s insightful and actionable feedback here. Australia Ageing Agenda also interviewed me following the charrette.
It won’t go away
Advertising and marketing images depict residential aged care facilities as bright and cheerful, and populated by happy fulfilled residents. Most do provide a high level of care and are caring yet 96% of Australians point blank refuse to entertain the idea of moving to a nursing home.
Some people are actively obstructive, even when presented with the imperative, when they can no longer care for themselves independently. This fact alone may be why we should rethink residential aged care in Australia.
Most of us never want to be, and never will be, in the position of being a resident of an aged care ‘facility’. We want to live a meaningful life until we take our last breath. However, many of us will experience the need for some level of support before death.
But no-one wants to be confronted with the prospect of the central artefact of our lives being a plastic-covered mattress, while handing over our banking details and paying hundreds of dollars a day for the privilege. We do what we can to avoid even thinking about it.
Yet thinking about it is precisely what participants had to do during the ‘Feels like Home’ charrette for the DMA/UQ Longevity by Design Challenge 2021.
In the design process I led as facilitator, architects and aged-care managers alike were taken out of their comfort zones to question their accepted knowledge of the Australian aged care ‘system’ and their long-standing experience of prevailing aged care architectural typologies.
By identifying directly with their own attitudes toward growing older, charrette participants uncovered so many things we take for granted in residential aged care designs that are not at all like ‘home’.
Step 1: what will matter to me when I’m older?
The workshop’s first step in overcoming the existing status quo was for the individual participants to imagine themselves as 85 year olds. What lifestyle would they want? What would they do in their typical day or week? Who is their ‘tribe’? What makes home ‘feel like home’?
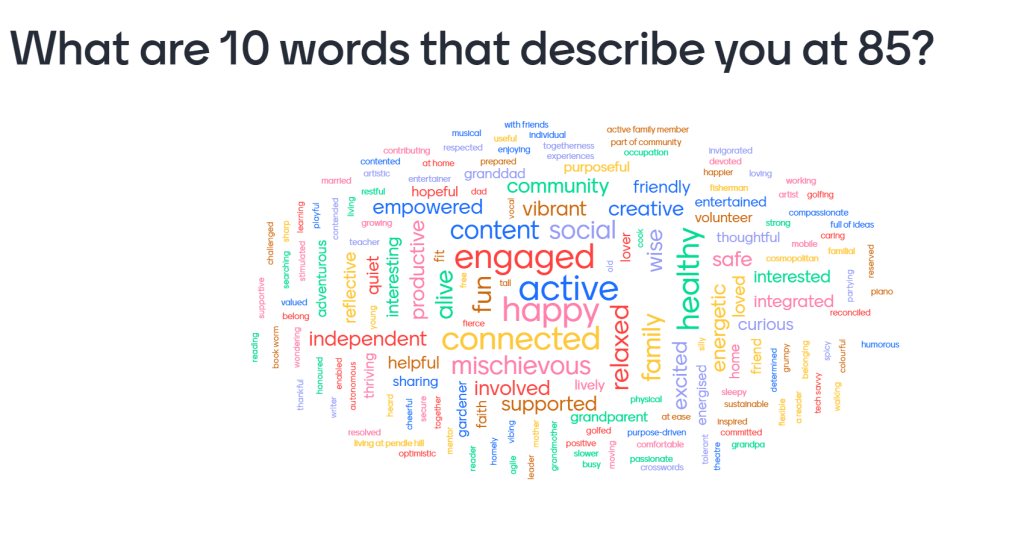
These insights into what will matter to us when we are older revealed the sense of ‘self’ we derive from engaging and connecting with the living world, according to a rich spectrum of individual values and preferences. We also derive sense of ‘self’ from our home as the private setting of personal identity and significant relationships.
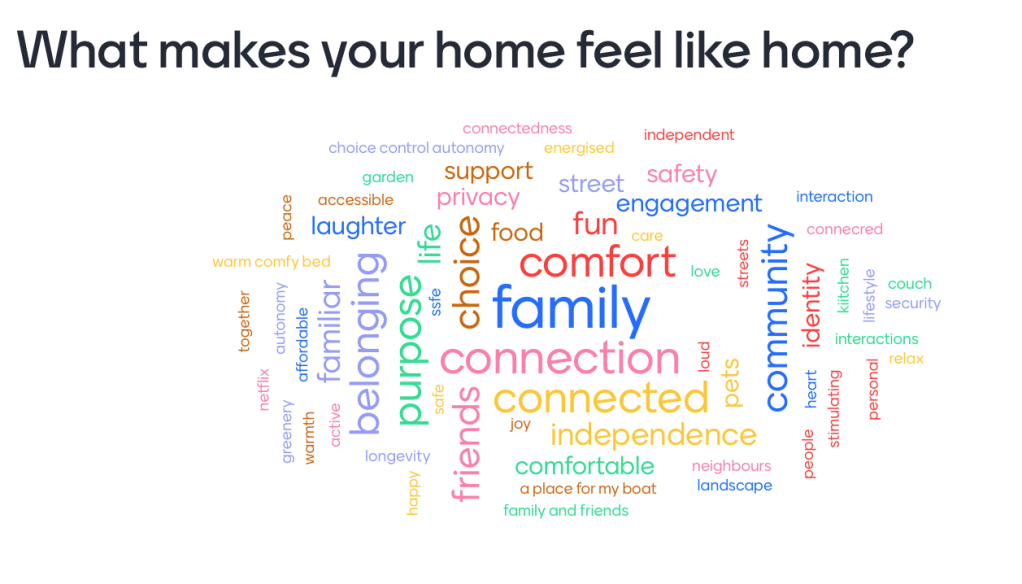
Participants’ pictorial and textual sketches of what home means to them brought out human needs that are important: interactions with other people, and connections with other living things, including plants and animals; activities and skills that bring joy and achievement; personal objects that are meaningful; a favoured prospect within and from the home to the world outside.

Step 2: What is the difference between a residential aged care ‘home’ and ‘home’?
Next, the workshop participants uncovered things we take for granted in residential aged care (RAC) that are not at all designed like ‘home’.
You have been disconnected
For example, RAC is often an isolated use set apart from the surrounding city. Despite attempts at a residential aesthetic, it is unable to shake off an institutional aura. A home has a front door and is connected to the outside world. A room in RAC is likely to open to a dead hospital-like corridor.
The COVID-19 pandemic accentuated the difference between a care ‘home’ and a real ‘home’. In pandemic-induced lock downs, unlike the rest of us, residents aren’t able to come and go from their home for any reason. [Aged care homes are neither home, nor hospital. They are not classified as health care buildings under the National Construction Code so lack the critical controls against airborne infection required of actual health care buildings.]
The social life of an aged-care resident
The people who live there are mostly all in the same age group but may not have anything else in common. The company of like-minded people, regardless of age, contributes to enjoyment of life. Interaction with staff members rather than friends and family is the norm. Every day is ‘ground hog day’. This observation shone a torch on how lack of things to do, often coupled with lack of mobility, feeds a vicious cycle of frailty.
Generation share
Your bedroom in RAC may have at least one other resident. And you are unlikely to be related to them – how come you are suddenly sharing with a roomy now that you’re old? The dining room might be large enough for about 80 people, so meals are taken amongst many strangers rather than around the household table.
What’s on the menu?
Meals are generally pre-prepared, and follow a schedule of food service. At home, we are involved in choosing meals and making food. A kitchen enables choice.
At home, we act with our own agency
The language we use to frame residential aged care concepts is disempowering. ‘Caring’ is something that is done ‘to’ or ‘for’ a resident in a ‘facility’ and assumes that one can do nothing at all for themselves, and can contribute nothing to others.
We are living longer and most of us plan to stay active, contributing to our family and the world around us. No-one wants or plans to have significant support needs or to spend our last years or months segregated from our community, tucked away with ‘old’ people in a place to die.
If aged care is not ok for young people why is it ok for anyone?
The national campaign for young care argues that “young people with high physical support needs deserve to feel at home – and free to live equally – in their community” through supportive accommodation and services. Yet for older people with high support needs, our society assumes that aged care is appropriate. If aged care is not ok for young people, why is it ok for anyone?
Why challenge the aged care paradigm through design?
Challenging everyday thinking is important for driving cultural and structural change that will benefit each of us as we age. Changing our expectations and language around residential aged care and design serves as a change agent for turning constraints into opportunities; inabilities into capabilities, and care into empowerment.
New thinking is needed to create supportive living environments for people to live their lives. The Longevity by Design Challenge provided a starting point to visualise what change looks like. This is precisely what we need to do in order to change what most people think is an intractable problem.
The dominant model of residential aged care doesn’t appeal to anyone, young or old, and for good reason. The physical environment is part of a systemic problem. Resembling either a hospital or a hotel, but not what we think of as ‘home’, out-dated or inappropriate buildings negatively impact residents’ quality of life.
A vicious cycle of accommodating people in hospital-like wards and depriving them of autonomy and meaningful purpose, leads to more frailty and cognitive decline, and justifies the need for hospital wards. People are kept alive through clinical care in hospital-like wards instead of real homes. Their basic physical needs may be met, but reasons to live are not.
Any one of them could be any one of us – who wants to live like that?
It is up to all of us to overhaul a system that is not working.
As a process of time, young people become old people. Instead of accepting the current status quo as the last resort for some ‘other’ members of society, the human centred approach recognises that another’s vulnerability is everyone’s vulnerability. It is up to all of us to overhaul a system that is not working.
Instead of hoping for the best, we can begin to build a picture of residential aged care that feels like home. Eventually the dial might move further where we look beyond the idea that people have to move from their community at all.
The ideas developed at the Longevity by Design 2021 workshop are a significant step toward community-integrated aged care. We all have more to do in creating environments that enable and support all of us to ‘live’ up until our end of life.


